SHOP DRY EYE CARE TODAY!
Use code VISIONARYEYE20 at checkout for 20% off!
Few developments in the field of ophthalmology have been as revolutionary as the advent of LASIK eye surgery. Originating from the groundbreaking surgical innovation of photorefractive keratectomy (PRK), LASIK (Laser-Assisted In Situ Keratomileusis) represents a quantum leap in refractive surgery. Today, we at Visionary Eye Center in Reno, NV, invite you on a journey to understand LASIK better and put your safety concerns to rest. Visionary Eye Center is a premier eye care center when it comes to completing the LASIK procedure in Nevada.
The history of refractive surgery is a compelling narrative of innovation and refinement. The early days saw procedures like radial keratotomy that, despite being pioneering, had their fair share of limitations. The game-changer came in the form of PRK and LASIK, both of which utilize a laser to reshape the cornea—the transparent front surface of the eye.
While both procedures utilize similar technology, they differ in their methods. In LASIK, a hinged flap is created on the cornea, folded back, and the laser is used to reshape the underlying corneal tissue. Post-treatment, the flap is repositioned, serving as a natural bandage. This allows for quicker visual recovery compared to PRK, where the laser is applied directly to the corneal surface, necessitating a longer healing period.
LASEK (Laser Epithelial Keratomileusis) is another variant that marries elements of both LASIK and PRK. The procedure involves the gentle displacement of the corneal epithelium before the laser treatment, which is then repositioned, often resulting in less postoperative dryness compared to LASIK.
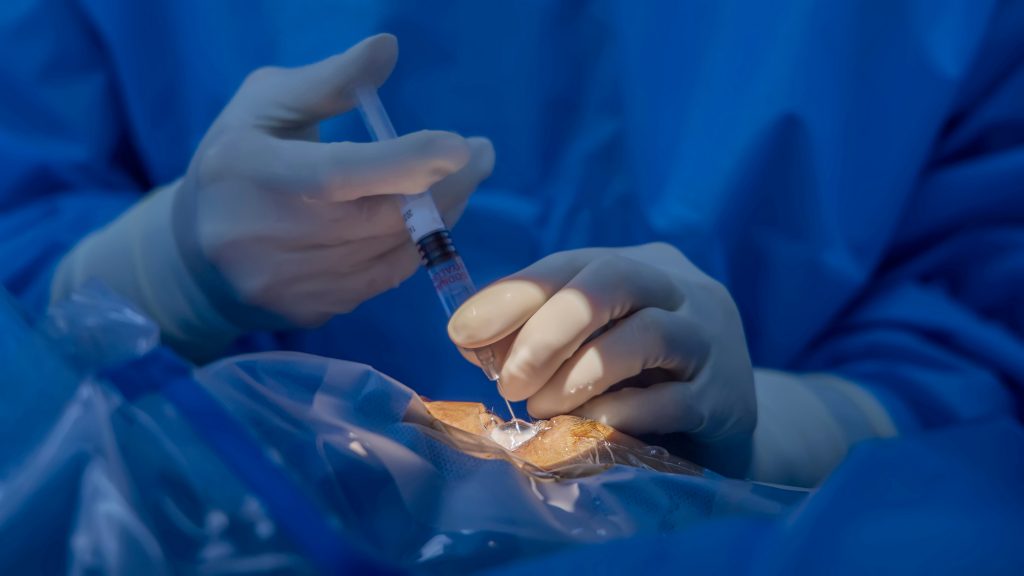
While LASIK has reshaped the landscape of refractive surgery, it may not be the ideal solution for everyone. For patients with high prescriptions or thinner corneas, or for those uncomfortable with the permanent removal of corneal tissue, an ICL (Implantable Contact Lens) is a practical alternative. This procedure involves placing a small lens between the iris and the natural lens of the eye. Importantly, the ICL procedure is reversible, causing minimal trauma to the eye.
Patients aged 40 and above, referred to as presbyopic patients, have other alternatives. One of them is the use of corneal inlays, such as the Kamra or Raindrop, which are inserted into the cornea. They create a pinhole effect, extending the eye's depth of focus and enhancing near vision. Another option is refractive lens exchange, which replaces the eye's natural lens with an intraocular implant lens. This procedure is akin to cataract surgery, with implant lenses capable of being tuned for distance, monovision, or even multifocal options.
For those reluctant about surgical correction, orthokeratology offers an effective, non-surgical route. This involves the use of specially designed gas permeable contact lenses worn during sleep that temporarily reshape the cornea, providing clear vision during the day without the need for glasses or contact lenses.
Visionary Eye Center are the premier eye doctors in Reno. We believe each person's visual system paints a unique view of the world, and thus, their vision correction solutions should be tailored to their individual needs.
Our practice prides itself on independence. As a standalone entity, we offer a personalized experience, ensuring a one-on-one relationship with our doctors. We fuse this old-fashioned, trust-based doctor-patient relationship with cutting-edge technology and contemporary treatment options, giving you the best of both worlds.
Education is empowerment. Following this philosophy, we strive to inform our patients about their treatment options, helping them make the most educated decisions about their care.
At Visionary Eye Center, we are committed to delivering unparalleled eye care using state-of-the-art, patient-friendly procedures like LASIK in Nevada. The evolution of refractive surgery demonstrates significant strides in ensuring safety and efficacy in vision correction. Whether you're considering LASIK or exploring other options, our team is ready to guide you every step of the way, taking care of your eye care needs while putting your safety concerns to rest.
Imagine a world where you can wake up to clear, crisp vision without reaching for your glasses or stumbling to insert contact lenses. This is the world of laser eye treatments, a revolutionary set of procedures that can transform the way you see — quite literally. Let me, Dr. Bolenbaker from the Visionary Eye Center, be your guide on this transformative journey.
To comprehend where we stand today, let's cast a brief glance at the history of refractive surgery. The revolutionary shift occurred with the emergence of PRK and LASIK, which swiftly replaced radial keratotomy, enhancing safety, predictability, and stability in vision correction.
Both LASIK and PRK utilize the precision of a laser to reshape the cornea. But, like two paths diverging in a forest, each carries its distinct approach and advantages. LASIK crafts a flap on the cornea that's folded back during surgery and repositioned afterward, speeding up the recovery process. PRK, on the other hand, works directly on the cornea, making it particularly beneficial for those with high prescriptions or thinner corneas.
LASEK brings together the advantages of both PRK and LASIK. This procedure delicately lifts the epithelium, treats the cornea, and then repositions the epithelium, thereby minimizing post-operative dryness. This fusion of LASIK and PRK methodologies offers a balanced solution for those seeking comfort and clarity.
What if you could enjoy the benefits of refractive surgery but retain the option to reverse the procedure if needed? That's exactly what ICL offers. By placing a small lens between the iris and the natural lens of the eye, this method allows for significant vision correction with the advantage of reversibility. This can be particularly appealing for patients with high prescription levels or those who may need to adjust their vision correction in the future.
With age comes wisdom, but also presbyopia, the natural loss of near vision that occurs typically after 40. However, procedures like the corneal inlay or refractive lens exchange offer effective solutions. The Kamra or Raindrop inlays create a pinhole effect, extending the depth of focus of the eye, thereby restoring near vision. Alternatively, a refractive lens exchange replaces the eye's natural lens with an intraocular lens, allowing for customized vision correction.
For those hesitant about surgery, orthokeratology offers an innovative alternative. By wearing specially designed contact lenses overnight, the cornea is gently reshaped, enabling clear daytime vision without the need for glasses or contacts. This non-surgical approach can be a game-changer for those who desire vision correction but are apprehensive about surgical procedures.
Nestled in the vibrant city of Reno, Nevada, Visionary Eye Center stands as a beacon of excellence in the realm of laser eye treatments. Known for its progressive spirit and dedication to cutting-edge medical advancements, Reno offers an ideal backdrop for those seeking the highest quality of vision care.

At Visionary Eye Center, we are dedicated to providing exceptional care and unmatched expertise in laser eye treatments. Our team, led by the esteemed Dr. Bolenbaker, consists of experienced professionals who are passionate about transforming your vision and enhancing your quality of life. With a commitment to excellence, we ensure that our patients receive the highest standard of care throughout their treatment journey.
We understand that your vision needs are as unique as you are. That's why we take pride in offering personalized treatment plans tailored to your specific needs and visual goals. We believe that clear vision is not just a luxury, but an essential asset that has the power to enhance every aspect of your life.
Whether you're considering LASIK, PRK, ICL, or any other laser eye treatment, we invite you to embark on your personalized journey to clear vision at Visionary Eye Center in Reno. From the moment you step through our doors, our friendly and knowledgeable staff will be by your side, providing guidance, answering your questions, and addressing any concerns you may have. We are dedicated to ensuring that you have a comprehensive understanding of the available options, empowering you to make informed decisions about your vision.
Your vision is our top priority, and we are committed to helping you achieve the clear, vibrant world you deserve. Contact our Reno eye clinic today to schedule a consultation and take the first step towards transforming your vision. Let us be your partner in this exciting journey towards a brighter future.
In the heart of Reno, Visionary Eye Center offers a pathway to a future where the world is crisp, vibrant, and free from the constraints of glasses or contacts. Unlock the potential of your vision and experience the transformative impact of laser eye treatments. Contact our Reno eye clinic today, and let us help you embark on a journey towards a clearer, more vibrant world. Your vision, empowered.
Today, we aim to unravel the artistry and thoughtfulness that goes into selecting the perfect frame shape to flatter your unique facial structure and personal style. Here at Visionary Eye Center, we hold firm to the belief that eyewear goes far beyond mere necessity, especially when it comes to Reno family eye care. It's a powerful tool to express one's personality, individuality, and style. Therefore, the importance of choosing a frame shape that complements your facial features and aligns with your fashion sensibilities with a Reno optometrist cannot be overstated.
To embark on this path, the first pivotal step is gaining a sound understanding of your face shape. Much like an artist who must comprehend the shape of their canvas before they can create a masterpiece, the shape of your face plays an integral role in determining which frame style will be the most flattering and suitable for you. Recognizing this is the cornerstone of making an informed and stylish decision when it comes to your eyewear.
There are five primary face shapes that most of us fall into, each with corresponding frame styles that accentuate their unique characteristics. Before we dive into the ocean of fashionable frames that await, let's take a moment to outline these five main face shapes. This crucial knowledge will serve as your compass, guiding you towards the frame styles that best harmonize with your natural features. We'll cover each face shape in detail, explaining their distinguishing traits and suggesting frame styles that lend themselves to each. This combination of understanding your face shape and recognizing the frame styles that correspond is the first step in your journey towards finding the perfect eyewear.

An oval-shaped face, marked by a forehead that is slightly wider than the chin, and characterized by high cheekbones, is considered the epitome of versatility in terms of frame compatibility. This face shape can pull off a myriad of frame styles with elegance. However, it is recommended to sidestep frames that are excessively oversized or bear harsh angular features. Round, square, and rectangular frames with softer edges enhance the symmetry of an oval face, accentuating its naturally balanced proportions without making it appear overly elongated or round.
A round face is characterized by its soft, curved lines, where the width and length of the face present in almost equal dimensions, creating a circular appearance. To counterbalance the roundness and bring about a sense of definition and elongation to your face, opt for angular and narrow frames. Frames bearing rectangular or square designs can provide the necessary contrast to the face's soft lines, imparting a striking balance and enhancing the facial features.
A square face is distinguishable by its strong, angular features, with a prominent jawline and broad forehead that make the face's width and length nearly equal. Frames that are round or oval can effectively soften the face's sharpness, injecting an element of balance to the pronounced angular features. Additionally, cat-eye frames and styles embodying curves can complement square faces by providing a pleasant contrast to the straight lines, giving an appealing and harmonious look.
A heart-shaped face, often recognized by its broad forehead and tapering towards a narrow chin, resembles the shape of a classic heart. This face shape can be balanced out by frames that are wider at the bottom, gently drawing attention away from the forehead. Subtle cat-eye shapes work wonders on this face shape, adding a flattering emphasis on the lower part of the face. Round and oval frames with thin rims can also harmoniously balance the wider forehead and narrower chin typical of heart-shaped faces.
A diamond-shaped face, marked by prominent cheekbones and a narrow forehead and chin, is uniquely attractive and somewhat rare. Frames with gentle curves can help to soften the angularity of this face shape and add balance, enhancing the overall facial symmetry. For this face shape, frames with wider temples can create an illusion of a broader forehead, adding balance to the face's dimensions. Designs such as oval frames and cat-eye styles accentuate the cheekbones and contour the face beautifully, resulting in a flattering and stylish look.
Now that we've explored the various face shapes and their matching frame styles, it's time to delve deeper into the next crucial stage - selecting a frame that not only complements your facial features but also resonates with your personal style. At Visionary Eye Center, our goal is to cater to every individual's unique style and provide some of the best family eye care Reno has to offer, we believe that your eyewear should be an extension of your personality.
In our extensive collection in Reno, optometrists carry an array of independent frame lines. What sets these frames apart is their ability to be customized. Each frame can be tailored to meet your specific needs, desires, and aesthetic inclinations, with diverse colors and shapes at your disposal. The capacity to personalize your eyewear ensures a perfect match with your style, further enhancing your distinctive look.
Now, let's delve into some popular frame styles that are making waves in the fashion world and are sure to capture the attention of those with a keen eye for style:

First soaring into popularity via pilots, aviator frames have since become a classic style staple that never seems to lose its charm. Traditionally characterized by a teardrop lens shape and a thin metal frame, aviators exude a sleek and sophisticated look. Not only are they known for their cool, casual vibe, but they also provide a flattering contrast to a variety of face shapes. Their larger lenses offer additional protection from the sun, making them a practical as well as a fashionable choice.
For those seeking a nostalgic nod to the glamour of the 1950s and '60s, cat-eye frames might be the perfect fit. These frames feature an upswept shape, often accentuated by bold lines and colors. Cat-eye frames manage to be both playful and elegant, adding a touch of vintage chic to any outfit. Their unique shape can emphasize your facial features and flatter most face shapes, particularly those with strong or angular features.
Championing a timeless, versatile style, round frames have been a preferred choice for both men and women over the years. These frames, known for their distinct circular shape, exude a sense of intellect and charm. They can range in size from oversized, which offers a more retro feel, to small and dainty, offering a more understated, contemporary appeal. For individuals with square or rectangular face shapes, round frames can provide a pleasing contrast.
For those who have a penchant for bold, edgy aesthetics, square frames are an excellent choice. These frames, as the name suggests, boast a rectangular or square shape and can add definition to the face, enhancing its natural structure. Their prominent lines and angles project a strong sense of style and confidence. They particularly complement round or oval face shapes by providing a striking contrast and balance.
Those who appreciate modern, minimalist aesthetics may find rimless frames to be their perfect match. As the name implies, these frames forego the traditional frame encircling the lenses, resulting in a barely-there, sophisticated effect. This understated style can accentuate the wearer's features without overwhelming them, suitable for individuals who desire a subtle, low-profile look.
Embarking on the quest to find that perfect pair of frames amidst a sea of shapes and styles can indeed seem overwhelming at first. However, having a clear understanding of your face shape coupled with a keen awareness of your unique style preferences equips you with the key tools to navigate this expansive realm with ease and confidence. You're not just on a quest for a practical solution to your optical needs, but also for a fashion accessory that speaks volumes about your personality and enhances your overall appearance.
We take pride in our diverse range of independent frame lines, each designed with a specific aesthetic appeal, and crafted to cater to the varied tastes of our discerning clientele. Whether you lean towards a timeless classic look, have a penchant for retro chic, or prefer the minimalist modern style, our extensive collection is bound to have something that piques your interest. But the selection process doesn't stop at the frames. Our team of Reno optometrists is on hand to provide expert advice, guiding you through this journey of discovery. Their experience and understanding of the intricate relationship between facial structure, frame shape, and personal style allow them to offer insights that can help you make the best decision.
We consider each customer's journey to find the perfect eyewear as a collaborative process, a partnership between you and our team. We take the time to get to know you, your preferences, and your needs, ensuring that you receive the best family eye care. Our clinic in reno ensures the frames you choose not only fit you perfectly but also resonate with your personal style. So, even though the task might seem daunting, you're not alone in your quest. Armed with your understanding of face shapes and frame styles, aided by our professional team, and powered by our wide array of stylish frame lines, you're well on your way to finding that perfect pair of glasses that not only meet your vision needs but also complement your personality and style. At Visionary Eye Center, our mission is all about transforming this journey into an enjoyable, enlightening, and ultimately successful experience.
Macular degeneration is a widespread eye condition that affects millions of individuals worldwide. Although it is most usually linked with older persons, it can also affect younger people.

Macular degeneration is a condition that affects the macula, the retina's center region. Because the retina is responsible for capturing information & transmitting them to the brain, any damage to this area might result in vision loss. The two types of macular degeneration are dry and wet, with dry being more common and less severe. Dry macular degeneration is characterized by macula thinning, which can result in hazy or distorted vision. Wet macular degeneration is more severe & can cause rapid vision loss due to the growth of abnormal blood vessels in the retina.
Macular degeneration can be a devastating diagnosis for anyone, regardless of age. This means that understanding the causes, symptoms, and treatment choices for this potentially blinding disorder is more crucial than ever for people of all ages. If you are concerned about developing macular degeneration, you can take steps & make a large effort to avoid it. Regular exercise, a healthy weight, and quitting smoking are also vital for your vision and overall health.
Macular degeneration can have emotional and psychological impacts on persons who suffer from it, in addition to physical symptoms. Losing your central vision might seriously impair your ability to accomplish daily duties and enjoy your favorite activities. It is critical to seek support from loved ones and to consider joining a macular degeneration support group. Your optometrist may also be able to identify services to help you manage with the disease's emotional implications.
There are various things you may do to assist control your macular degeneration in addition to working with your healthcare professional. One of the most important is to shield your eyes from UV radiation, as UV rays might hasten the condition's damage & overall speed it can progress at. This means wearing sunglasses or a hat with a brim when you are outdoors, and avoiding tanning beds and other sources of artificial UV light. Early detection and treatment can make a significant difference in preserving your vision. At our Visionary Eye Center, we offer comprehensive eye exams and specialized care for patients with macular degeneration.
Regular eye exams allow patients to keep track of their vision, take medicine that can slow the progression of their condition, and avoid serious vision loss. This is very crucial for those who have a family history of macular degeneration & are vulnerable to it due to other circumstances.
Aside from medical treatment, lifestyle adjustments can help minimize the incidence of macular degeneration. By eating a nutritious diet, not smoking, and protecting your eyes from UV radiation, you can improve your eye health & reduce your chances of having this condition.
Visionary Eye Center is dedicated to assisting our patients in maintaining good vision & preventing the beginning of eye illnesses such as macular degeneration. Together, we can work towards protecting and preserving your vision for a lifetime. Contact us today to schedule your comprehensive eye exam and learn more about our services.
Schedule an Exam with a Nevada Optometrist
Astigmatism is a common eye condition that affects many people. It occurs when the cornea or lens of the eye is misshapen, causing blurred or distorted vision. If you're experiencing symptoms of astigmatism, such as blurry vision, headaches, or eye strain, it's essential to see a Nevada optometrist.

Astigmatism is a refractive error that occurs when the cornea or lens of the eye is irregularly shaped. Instead of being round like a basketball, the cornea or lens may be more oval, causing light to be focused unevenly on the retina. This can lead to distorted or blurry vision, making it difficult to see objects clearly at any distance. Astigmatism can occur on its own or in combination with other vision problems, such as nearsightedness (myopia) or farsightedness (hyperopia). Astigmatism can occur in both adults and children, and it often develops early in life. Some people are born with it, while others develop it later in life due to an eye injury, surgery, or a disease like keratoconus. Astigmatism can also be caused by certain genetic conditions or diseases like diabetes.
Fortunately, there are several ways to treat astigmatism. The most common method is to wear glasses or contact lenses that correct the irregular shape of the cornea or lens. These lenses are specially designed to compensate for the uneven curvature of the eye, allowing light to be focused properly on the retina.
Another treatment option is LASIK eye surgery, which uses a laser to reshape the cornea and correct the irregular curvature. This is a more permanent solution than wearing corrective lenses, but it is not suitable for everyone. Your eye specialist in Reno, NV can help you determine whether LASIK is the right choice for you.
At Visionary Eye Center, we understand the importance of proper eye care and the impact it can have on your daily life. Our experienced eye specialists and optometrists provide comprehensive eye exams, including testing for astigmatism, and offer personalized treatment plans to help you achieve optimal vision health. We also offer a wide selection of glasses and contact lenses to suit your needs and style preferences.
Astigmatism is a common eye condition that can cause blurry or distorted vision. It's important to see a Nevada optometrist to get the proper diagnosis and treatment for this condition. At Visionary Eye Center, we're dedicated to providing our patients with the best possible care and treatment options to ensure optimal vision health. Contact us today to schedule your comprehensive eye exam and learn more about our services.
Schedule an Exam with an Eye Doctor in Reno
Search for “Eye doctor Reno” and you’ll get dozens of results. Some are individual practices, and some are big box stores with walk in eye care centers. There’s nothing wrong with shopping around to find a good eye doctor. In fact, we encourage it. After all, you’re looking for a professional whom you’ll entrust your eyes to. And unhindered vision is a vital aspect of your overall well-being. Check out Visionary Eye Center’s tips on how to choose a good eye doctor:
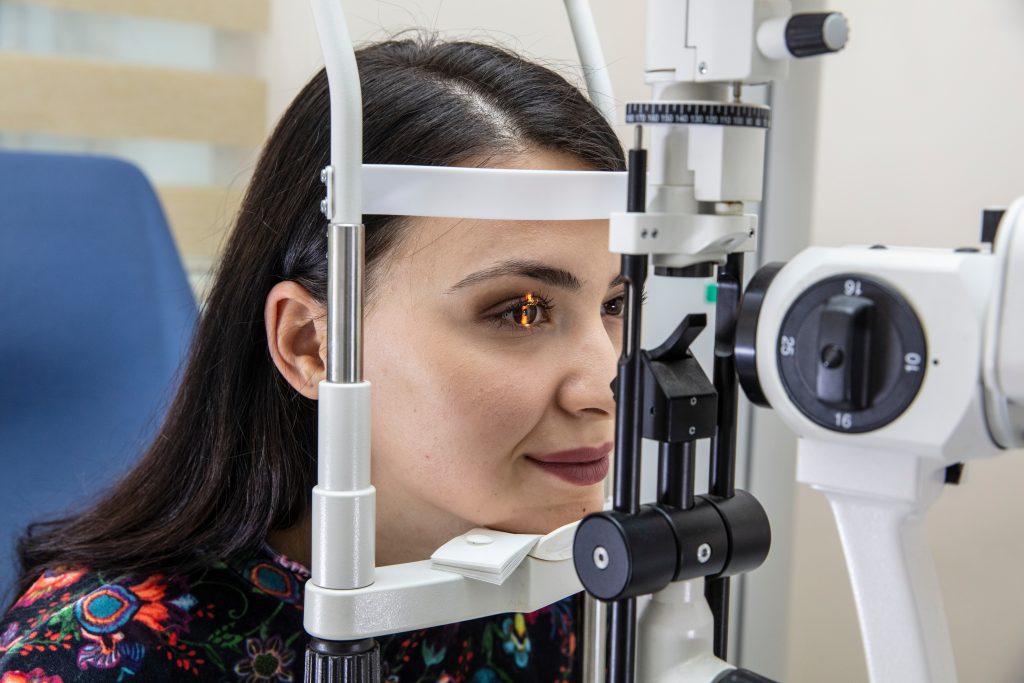
There are plentiful resources online that make it simple to compare optometrists in Reno, Nevada. Dr. Bolenbaker’s information can be found on helpful sites like healthgrades.com, where you’ll be able to get a general overview of the practice, as well as the accepted insurance providers.
A well-rounded education in optometry can indicate if a doctor has specialty training in various eye care disciplines. Dr. Bolenbaker found a passion for optometry at Washington State University. After completing over 100 hours of observation time (only 30 are required to pursue a degree), he went on to graduate from Pacific University’s College of Optometry in 2003.
While pursuing his Doctor of Optometry Degree, he was an active member of the Beta Sigma Kappa International Optometric Honor Society. Dr. Bolenbaker’s practice now offers general optometry services, but also specializes in areas like low vision, dry eye, myopia control, and orthokeratology.
From routine checkups to more advanced eye conditions, you want a doctor who’s experienced in providing high level care. The greater breadth of experience an optometrist has with treatments, the better your results are likely to be - both short and long term. It’s a good idea to ask if your doctor treats your specific condition, if you are aware you have one.
How many patients have they treated with glaucoma? Myopia? Lasik? Getting details on if they have experience with a certain condition before visiting can save you time. If you’re looking for a Reno eye doctor that specializes in several advanced treatments for you and your family, check out Dr. Bolenbaker’s services.
While the doctor of optometry is a very important factor in choosing a practice, remember that you’ll also be interacting with the front office staff and opticians. The staff should truly care about your well-being, and provide a seamless experience from check in to check out. The Visionary Eye Center staff consists of passionate Nevada eye specialists who are welcoming, knowledgeable, and caring. Our team includes experienced and energetic people whose goal is to provide the best eye care possible.
Checking out what others have to say about an optometrist provides an unfiltered glimpse into how a practice is run and what to expect on your visit. Look into the typical scheduling experience, office environment, wait times, and office staff friendliness. Another point to look for is how much time the doctor spends with patients, and their ability to inform patients on the treatments they are receiving. Visionary Eye Center prides itself on receiving great reviews from our valued patients. Check out what they have to say on our reviews page!
Choosing an eye doctor isn’t the most exciting thing, but it can make a huge impact on your ability to experience the things you love. Visionary Eye Center is a great choice for any Reno resident seeking a specialized optometry practice with the experience and care you have come to expect in a professional healthcare office. We are currently accepting new patients, so give us a call to set up an appointment.
Summer is winding down, and school is in full swing! It’s time for children to refocus their attention from summertime fun back to books and the white board. For some kids, that’s easier said than done. As a highly-rated pediatric optometrist, Reno has come to love, Visionary Eye Care Center can examine and help alleviate common conditions associated with classroom vision.
A comprehensive pediatric eye exam should be right at the top with pencils and paper on any back-to-school checklist. While your child may have visited their pediatrician or school nurse and had their vision screened, these exams are not comprehensive. Screenings can sometimes reveal potential conditions, but are not meant to diagnose vision problems.
A child's vision can change rapidly and sporadically from ages 6 to 18. Left unchecked, vision conditions can:
One of the most common vision conditions optometrists encounter in children is nearsightedness. The medical term for this is Myopia. Myopia occurs when the eye’s shape becomes elongated, distorting the image of far away objects (the whiteboard, sports balls, or friends on the playground), while nearby objects remain clear. It’s recommended to ask your child whether they are having trouble focusing on letters and numbers at the front of the class. If the answer is ‘yes’, it’s time to get them into the optometrist Reno, NV trusts in order to diagnose the cause and get them back to learning at their greatest potential. The sooner it’s diagnosed, the sooner that treatment can administrated.
If your child already wears glasses to treat the effects of myopia, there are options to slow its progression. We want to emphasize that under-correction, or giving your child a slightly lower prescription to “strengthen” the eyes will not help with myopia. This approach will only make them see things blurrier, and has been clinically disproved as a treatment. In order to help with myopia control, an optometrist will recommend one of the following methods:
Even if your child has not explicitly said that their vision is blurry when looking at the board, it’s never a bad idea to have it checked. Comprehensive eye exams can identify potential anomalies that screenings glance over. To diagnose and alleviate conditions like myopia, we encourage you to book an appointment with our knowledgeable practice. We’ll see you here, bright and clear!
Age-related vision issues can affect anyone over time, and may not be apparent right away. Even if you haven’t experienced vision issues during your life, some conditions can begin to surface when you’re 40 or older. At Visionary Eye Center, our Reno optometrist recommends the following tips to preserve your eye health:
After you turn 40, it’s important to receive an eye exam every year. This helps to record and track any changes that may affect your vision. If you are experiencing any of the following symptoms, we recommend consulting an optometrist to mitigate risks and provide treatment where necessary:

Like it or not, you become more susceptible to vision issues as you age, and some can be debilitating. From dry eyes, to cataracts, to macular degeneration, an experienced eye doctor can diagnose and produce a treatment plan to suit you.
Dry eye is more debilitating as you age. While it may seem common in Northern Nevada thanks to our dry climate, there may be other factors contributing to the symptoms of burning, redness and tearing. As many as 3 million women and 1.7 million men over 50 in our country are affected by the syndrome.
How does dry eye occur? Tear film dysfunction has many causes, including computer use, contact lens wear, makeup, hormone changes associated with aging and autoimmune disorders, which further increase the risk of corneal scars or infections.
Optometrists also see numerous patients with cataracts, the leading cause of blindness in the world. Cataract symptoms include a decrease in visual clarity, foggy vision, glare, and halos of light. Cataract surgery is a simple outpatient surgery and the artificial lenses placed during it will last for the rest of your lifetime.
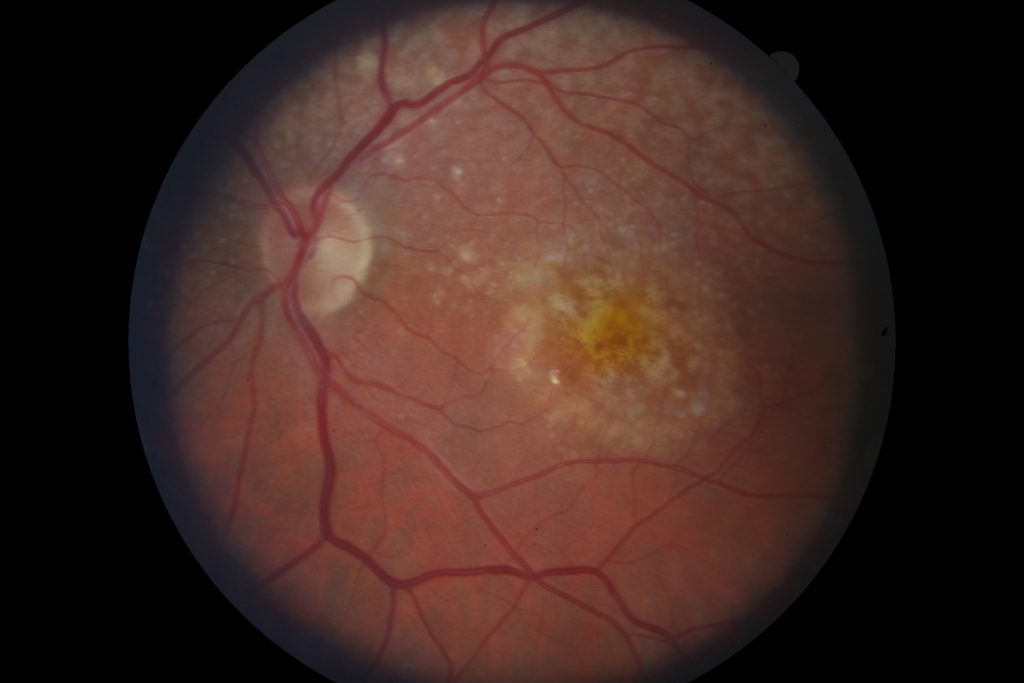
Retinal scan of dry macular degeneration
Lastly, macular degeneration is the primary culprit for blindness in adults over 50. While these patients never go completely blind from the condition alone, it certainly devastates their independence. There are two versions of macular degeneration: wet and dry. At Visionary Eye Care Center, we diagnose and manage both conditions with help from our local retinal specialists.
It turns out the advice of “don’t stare too long at the TV” is still true, thanks to our phones and other electronic devices. Recent studies show that we blink less than half as often when looking at a screen, which can lead to dryness and eye fatigue.
Our Reno family eye care experts suggest that everyone, at any age, should practice the 20-20-20 rule when using a screen. Just looking at something 20 feet away, for 20 seconds, every 20 minutes, will help reduce the dryness and eye strain of computer vision syndrome.
Using proper eye protection outdoors is also important. UV rays are harsh on your eyes in the long term. Sunglasses work wonders to protect your eyes from the elements and reduce your risks of cataracts, pterygia and macular degeneration.
Lastly, a balanced diet that is rich in Omega-3s, Vitamins C and E, and zinc, can help combat age-related eye disease. These supplements are often used to combat the effects of dry eye and slow the progression of dry macular degeneration.

All in all, simple changes to your lifestyle and new habits will help prolong your eye health. If you’re experiencing changes in your vision or have questions about how to protect your eyes, make an appointment at our Reno optometrist office today.
Request an Appointment at Visionary Eye Center
It’s pretty painful to get a sunburn after missing a spot on your skin with sunscreen. Just imagine how a corneal sunburn would affect your quality of life during some of the best weather of the year. Also known as photokeratitis, this issue occurs during short-term exposure to high intensity UV-B rays. Photokeratitis is painful but temporary and is similar to a sunburn, but on your corneas (the clear portion of your eye in front of your pupil) instead of skin. It can look like a yellow, thickened area in the whites of your eyes. Too much exposure with ultraviolet rays can temporarily damage your conjunctiva, which is the clear layer of tissue covering the inside of your eyelid and whites of your eye.
Summertime activities that can put someone at increased risk for photokeratitis include mountain climbing, hiking, skiing, and swimming. It can also occur if you use sunlamps and tanning beds, or spend time in an environment with consistent UV light exposure.
There are two types of UV light proven to contribute to eye, skin, or health issues. UV-A rays can pass through your eye’s cornea to reach the lens and retina. UV-B rays can’t pass through glass but still can cause eye damage.

The symptoms of photokeratitis are pain and redness in the eyes, swelling, light sensitivity, headaches, temporary loss of vision, twitching eyelids, and seeing halos (like in the photo below). They can last from six to twenty-four hours but typically disappear after forty-eight hours.

Photokeratitis is most often formally diagnosed after an eye exam, and your doctor will place drops containing a special dye known as fluorescein in your eyes to reveal any superficial irregularities on the surface of your cornea. As for treatment, go indoors immediately after experiencing symptoms and avoid bright lights. Once in a darkened area, place a cold washcloth over your eyes and take ibuprofen. If you wear contact lenses, remove them and use artificial tears to reduce discomfort.
The longer you were exposed to UV lights, the more severe the symptoms. Long term exposure to even the tiniest amount of UV radiation can increase the risk of developing a cataract or macular degeneration (an eye disease that leads to vision loss in the center), or cause tissue elevations on the surface. These conditions are known as pinguecula and pterygium, but can be prevented by wearing sunglasses.
If you wear contacts, ask about ones that absorb UV rays when working or playing in a sunny environment. But even with these types of contacts it’s still important to wear protective sunglasses to shield your eyelids and conjunctiva from the suns’ rays.

The good news is that photokeratitis is preventable simply by wearing the proper eye protection when outside, like prescription sunglasses or snow goggles in the winter. Glare from snow, sand, or water can cause burns to your eyes even if it’s overcast. A wide brimmed hat can help filter out the sun’s rays as well.
When purchasing a pair of sunglasses, it’s worth noting that not all sunglasses are polarized. Polarized sunglasses are manufactured in a distinctive way that creates a different pattern in the lens to block out more light than a usual pair of sunglasses. When choosing a pair, look for one that provides one hundred percent UV protection or UV 400 protection. Prescription sunglasses help with overall light sensitivity, headaches caused by glare, and regular eye strain from squinting in bright sunlight.
For more information, check out our other blog post on prescription sunglasses here.
Be sure to visit your eye specialist once a year to stay up on your eye health and catch any issues early. It’s never been a better time to make an appointment with the team at Visionary Eye Center to get the perfect pair of prescription sunglasses for your summer adventures.
Our Reno eye care facility is one of the best in preventing photokeratitis in our patients.
Schedule an Exam with an Eye Doctor in Reno
As the school year comes to an end, it’s important to make sure that your child’s eye health remains on track during the summer and beyond. Younger generations are more susceptible to myopia, which is caused by the lengthening of the eye from front to back. Consequently, light is focused in front of the retina and not directly on it, causing distant objects to be blurry. The best way to prevent child myopia from developing or worsening is to get them in to see a Reno optometrist who will create a treatment plan designed specifically for their eye needs.
Myopia is prominent in children today because of environmental factors ranging from poor lighting and not enough time outdoors to excessive screen time. Genetics also can play a role based on if both parents or only one is myopic. A fifty percent chance of myopia is possible if both parents have it, a thirty-three percent chance if one parent has it, and a twenty-five percent chance if neither parent is myopic.
Children who spend at least two hours a day outside with sunglasses on are less likely to become myopic. However, researchers found that once a child has become nearsighted, outdoor time does not slow myopia progression.
Myopia can put an individual at risk for complications like retinal detachment, glaucoma, cataracts, chorioretinal degeneration, and more as they age. It is definitely considered an epidemic with a forty percent diagnosis rate in young patients and climbing.
Another increasingly common issue in children today is eye turns, or strabismus. Known as being “cross-eyed,” it’s the result of excessive focusing. Sometimes it is a genetic issue in children, and other times it can be developed between the ages of one year to four years. We can detect and treat both of these issues with vision therapy and surgical treatments, all while ensuring you or your child have the proper depth perception.
The MiSight 1-day program is FDA approved and helps optometrists across the country change the futures of young patients on the road to myopia. According to CooperVision, the corporation behind the high-quality contact lenses, age-appropriate children wearing MiSight experience an average of 59% reduction in myopia progression during a three-year period. There’s also a 52% reduction in eye lengthening, and more than 90% of children continued to express a strong preference for MiSight 1-day contact lenses over their glasses at the five-year check-up. Their parents expressed the same sentiment as well.
We typically recommend MiSight for lower levels of myopia (approximately -1.00 or less), over alternatives like Ortho K for myopia control. If you’d like to learn more about the efforts to educate people and prevent worsening side effects of myopia, check out CooperVision’s Facebook page and YouTube channel.
Over half of the country’s eye care practitioners agree that if myopia is left untreated, it will lead to irreversible vision loss. After some time, detrimental diseases like retinal detachment or myopic maculopathy are possible. MiSight lenses accommodate a more active lifestyle, provide and correct distance vision immediately, and are comfortable at any age.
As a pediatric optometrist in Reno NV, Visionary Eye Center has plenty of experience helping children and even their parents navigate the different tests and procedures for evaluating vision and eye health. Here is a quick rundown of what some of the most common machines we use to treat myopia while lessening its side effects over time:
One of the machines our practice utilizes is the Zeiss IOLMaster for axial length measurements, as it’s the best way to monitor myopia progression. This equipment for ocular biometry measures the size of the eyeball, originally designed to calculate the dioptric power of intraocular lenses implants (IOLs) for cataract surgery, but is now used by leading myopia control doctors to track the growth of the eye.

This is something that can be easily monitored in children because when the elongation progresses beyond 26 millimeters, the risk of potential vision impairment increases dramatically. Even better, this machine is quick and painless – we can measure both of a patient’s eyes in less than a minute!
Measuring axial length is a vital measurement when looking at treatment, as using prescription alone is too variable. Unfortunately, many doctors haven’t equipped their offices with the technology at this time– but we have it here at Visionary Eye Center, setting us apart as experts treating myopia at a higher level.
Measuring axial length is also the only way to track myopic elongation in orthokeratology. Orthokeratology, or Ortho-K, creates specially designed corneal molds to considerably reshape the eye overnight as part of an FDA-approved process for all ages. Similar to how dental braces can reshape your teeth, Ortho-K processes help fix those refractive errors that cause myopia or hyperopia and astigmatism as well.

Topography maps are taken using our Keratograph 5M and are used for fitting contacts like MiSight, as well as dry eye testing with the Crystal Tear Report. It’s an incredibly helpful tool for the diagnosis of and education about dry eye. As an advanced corneal topographer, the Keratograph can examine the meibomian glands in infrared imaging and evaluate the tear lipid layer. The Keratograph is effective in measuring the tear film break-up time and the tear meniscus height measurement in a non-invasive, painless way for patients.
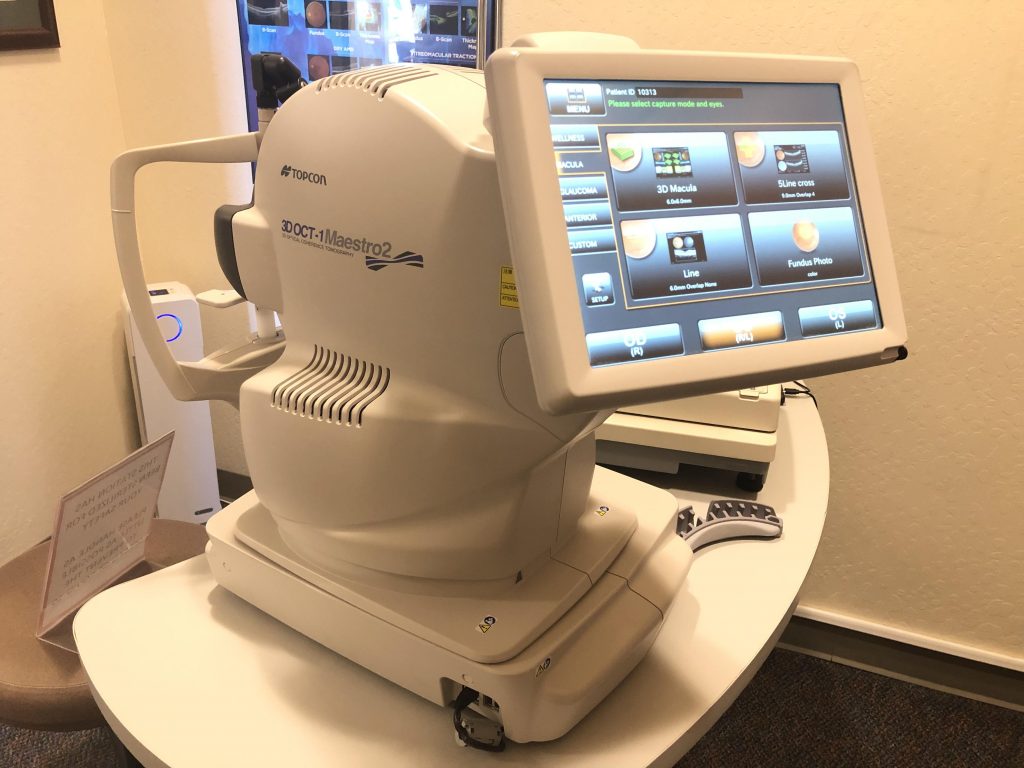
The Maestro is used for the screening of glaucoma, cataracts, diabetic retinopathy, and macular degeneration. Taking a look at a patient’s retina, optic nerve, and anterior segment of the eye is a much quicker practice than before. Using Maestro technology allows our Reno optometrist to rapidly and clearly analyze various functions and facets of the eye for the most reliable results.
The team frequently relies on Pentacam technology to custom design gas permeable (GP) and scleral contact lenses. Gas permeable contacts are made of firm, durable polymers with high oxygen permeability. High oxygen permeability helps keep eyes healthy with orthokeratology for myopia control or scleral lenses. The Pentacam allows our Reno optometrists to create a 3D model of the front surface of the eye which can be used to design highly customized contact lenses.
All in all, we strive to have the best technology for our patients and the services and scans provide vast treatment options. If you’re struggling with myopia, dry eye, or the after-effects of either of these conditions, Dr. Jason Bolenbaker is here to help.
All in all, we strive to have the best technology for our patients and the services and scans provide vast treatment options. If you’re struggling with myopia, dry eye, or the after-effects of either of these conditions, Dr. Jason Bolenbaker is here to help.
The MiSight program is just one of the ways we reach our goals based on our philosophy of how an educated patient makes better health decisions for their families. We want our patients to be educated on every treatment option offered to them, and make the best choices for their care.
Our team of optometrists in Reno is ready to help patients of all ages begin their eyesight correction journey and prevent any further issues. Contact the Visionary Eye Center today and make an appointment with a medical care team you can trust.
 775.827.1100info@visionaryeyecenter.com8175 South Virginia Street Suite B-900
775.827.1100info@visionaryeyecenter.com8175 South Virginia Street Suite B-900